The Beast is Back, Professor Vogl and Anne Boleyn
/No nose stud - first time in nearly 30 years
I have been concerned that the cancer was on the move for a while, ever since one of my liver enzymes (GGT - a marker of inflammation) started to rise. Over the summer the rise was slow, but it has been steady. The bloods taken after my ovaries were removed had it at 116 (normal is under 40) - which pretty well confirmed I was going to have to take action soon. I was determined to go to Tanzania and had a letter from my oncologist for the insurance which simply stated that hehad examined me in September and that at that point I was fit and able to travel to ‘Africa’. Which at that point was true. But things change. Before even going to Tanzania I had arranged (with help from Grace Gawler who runs a foundation to support people navigate cancer options) to go to Professor Vogl in Frankfurt.
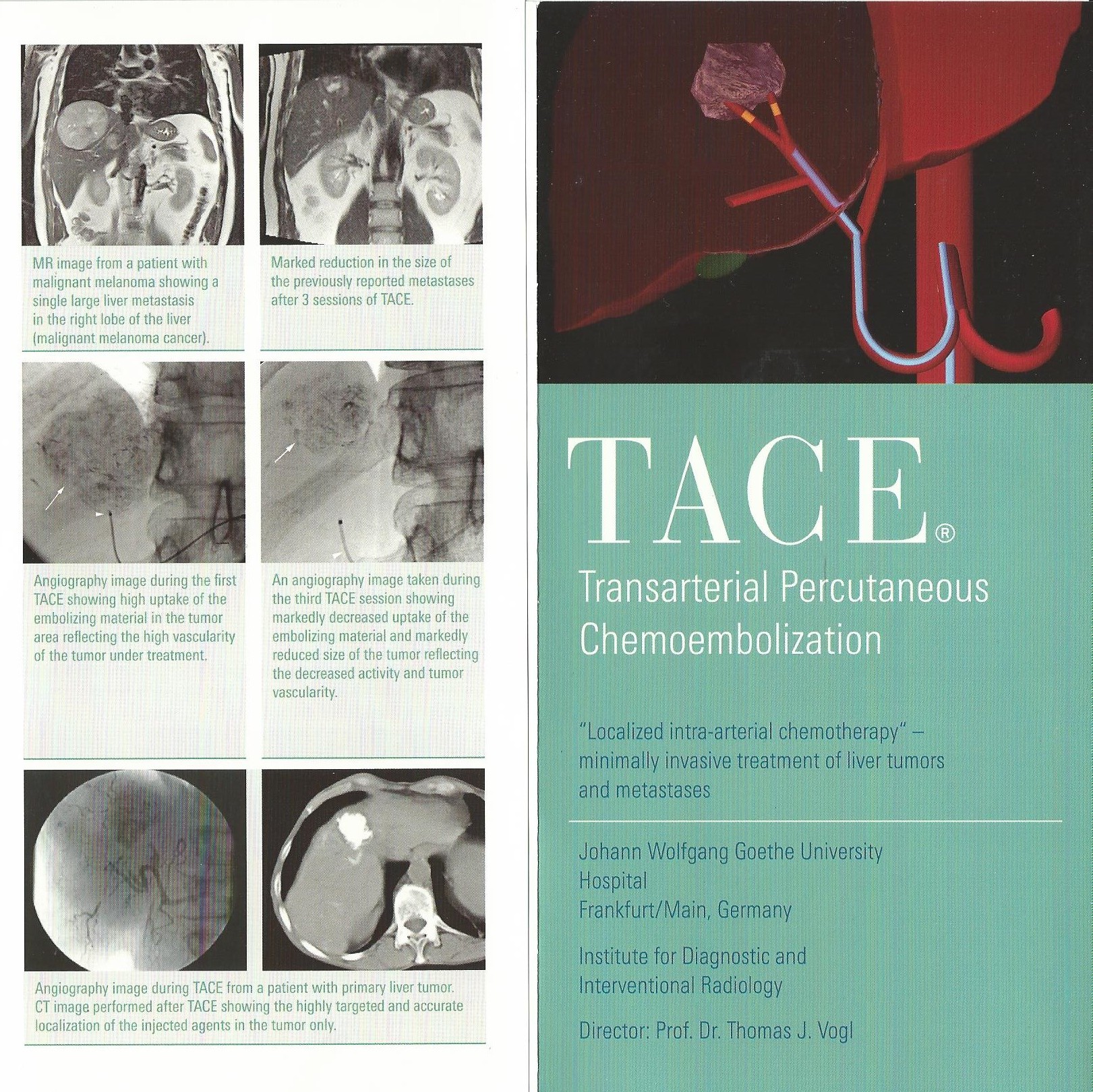
Prof Vogl is an interventionist oncologist (aren’t they all?) and he is an expert at stabilising tumours and reducing tumour load in major organs (I am sure he describes himself very differently but this is my understanding). In the old days if the cancer had reached the liver the approach was more or less, bad luck, sorry there is nothing much we can do. Nowadays they are working out ways to try and keep you alive longer, with less toxic treatments so you have some quality of life - but they still approach different cancers differently. If you have primary liver cancer a very normal treatment is something called TACE - or transarterial chemoembolisation. Which to you or I means - chemotherapy injected via the hepatic artery to the blood supply to the tumours, and then embolisation means something like - and block it off so the chemo can't escape and the blood supply to the tumours is cut/reduced. I have attached a leaflet that describes it much better. For those with primary liver cancers a good 66% respond well and the tumours can be stabilised or pushed back for 10-14 months and if they are in good enough health then they can have it again and again even. This really can extend life for this group and can keep them going until they can get a liver transplant.
For those of use for whom the cancer is secondary i.e. it originated somewhere else - in my case the breast, TACE does not seem to be considered in the UK. Presumably because they reckon that the cancer is already out the bag and so it is money down the drain. But for those of us for whom the cancer has remained (touch wood this is still the case) in the liver since secondary diagnosis it would seem sensible to more directly target the chemo to the tumours there (if they are under control they can't kill me) and in doing so reduce the impact on the healthy cells in the rest of my body. I knew that my options in the UK when it started progressing consisted of either an IV chemotherapy or a hormone approach, probably the IV chemo however, as once it is on the move in the liver you need to get it under control pretty sharpish and then try aromatase inhibitors (hormone treatment for oestrogen positive cancer). The IV chemo reaches the liver via the portal vein but the tumours in the liver are usually fed by the hepatic artery. SO if you inject the chemo directly via the hepatic artery you can use lower levels of chemo with much greater effect. And
Prof. Vogl is top of his game. He not only does this for livers but lungs and other places. He also has a number of other approaches to reduce tumour load. In my case the tumours are spread over both lobes of the liver which rules out some approaches. Eg - resection - were I to have one or two clear tumours the liver could potentially be resected - i.e. the bit with the tumours cut out. As livers are so resilient (got to look at the positives) the liver will regrow. I had investigated this last time my liver got bad, but the treatments then worked so well I did not need to follow it through. This time it was the obvious next step. Only one part of the plan, as I do still need some systemic treatment as the cancer, even if not yet visible, is still around my body and so I will need some treatment to keep this also at bay. Having the tumours in the liver got under control (this is the plan) may then mean I can start on a aromatase inhibitor, perhaps a low dose chemo or an immunotherapy.
So plan get tumours under control is underway. This means money. About £5000 a visit (euro 3900 plus flights and hotel for me and someone to accompany me) a go. I will need 2-4 treatments of TACE because they can only do one lobe at a time and unless they get a spectacular response first go they are likely to need at least one follow up treatment. The treatments are every 4 weeks.
We (my longest best friend came with me) arrived in Frankfurt (flights to Frankfurt are not cheap) and stayed in a hotel relatively close to the Frankfurt University Hospital. We reported at 7.30am in time for an 8am appointment. I had been warned that Prof Vogl has a slightly distracted manner so this, which I can confirm is true, did not bother me. The University Hospital is on an enormous site and there was quite a factory production line feel about the process. The Department clearly deal with hundreds of patients a week which I suspect affects their capacity to make any one feel individual. This did not mean they were unkind, more robotic in their smiles and responses.
After a brief meeting with Prof. Vogl and payment for the procedure I was sent to have an MRI of my liver. This involved being escorted down corridors to a line of numbered doors, or cubicles as it turned out, each with a door to enter, a locker for personal belongings and another door on the other side which then led to a corridor to the MRI room. I entered door 11, removed all my clothes and jewellry. This included my nose ring, as MRI’s have magnets which would attract metal.
I have not removed my nose ring since the year I had my nose pierced. I had it pierced aged 18 in 1989 (I was ahead of the crowd) in Bangalore South India during my gap year before going to university. I chose a local nose piercer, not wanting a more techno piercing with a gun. I reckoned that with so many millions of indian women having nose rings the traditional approach would be safest. This involved a sharp curved piece of metal which was inserted manually. I remember, in my attempt to protect myself from infection, pulling out a little bottle of surgical spirit that I travelled with and requesting that the old man (he probably was not that old but at 18 over 40 looked pretty old), clean his hands and the equipment with it. I was travelling with a friend who was also going to have her nose pierced, but was less convinced so I had offered to go first. I knew if I made too much fuss she may back out so held in the screech of pain that should have accompanied the actual piercing (although I could not hold back the spontaneous tearsfrom the pain that filled my eyes). Forcibly smiling after the event I reassured my friend that it wasn’t that bad really. She certainly did not hold in the screech of pain which was loud and came with much swearing. But it was over fast and we went away with rather throbbing noses and gold plated studs. Being sensitive to most metals mine became red and aggravated so I went to have stud of real gold and a tiny diamond made up. I reckoned that I would not easily be able to buy nose studs in the UK in those days. I have worn this nose stud every single day since then. I could never work out how to take it out and feared that if I tried I would either break it, lose it or not know how to put it back in. A number of times during my life I have been challenged to remove it. Once I turned up for a waitressing job in my early 20s at the Queens Club in London, and they asked me to remove it, which I refused to do and was then told to leave. But my nose stud meant too much for me compared with that one off waiting job. When having operations and CT scans I have been asked to remove it, but when I have said I cannot they have simply covered it with a plaster. I had always thought I would take it out by the age of 30 (which then seemed ancient) as I considered it might stop people taking me seriously. My thirtieth birthday passed and I kept it in. Soon after I was interviewed for a job at Brighton and Hove Council. My children were very young and I really needed a local job to help me manage the children and enable me to finish my PhD (which meant needing money to pay huge child care costs). I remember seriously considering if this was the time I had always imagined, when I needed to grow up and take it out in case it affected my chances of getting the job. But I couldn’t bring myself to do it and walked into the interview room. I was at that time 7 months pregnant with William which was probably far more likely to affect my chances of being employed than a nose stud. And there, there sat the woman who would become my boss, herself with a nose stud. We do live in Brighton, so this should not have been such a surprise, but even then nose studs were far less common than nowadays.
Below - me in my hospital gown and no nose stud and me at 18 in India the year I had my nose pierced
Anyway, this was my first MRI scan and clearly the risk of the magnets attracting my nose stud gave me very little choice. I simply had to remove it. I had seconds to do so and was all in a fluster ready to mourn the loss of this little friend in the event I had to break it to get it out, but was surprised that it was a relatively straightforward affair. What was far more likely was that I would then lose it as it is really very tiny and I had no special case to put it in. I put on the standard, do up at the back hospital gown and came out the other side of the cubicle, locked the door shut and waited to be escorted to the MRI scan. An MRI is also a polo like round shape but the hole is much smaller so when they wheel you in it feels very claustrophobic as everything is so close. It makes a loud clanging sound when it starts working. It took about 10 minutes in this position. I am not claustrophobic but it is difficult not to feel anxiousin this position so I started my distraction techniques. Strangely what came into my head was Anne Boleyn. I read a book last year about her last weeks before she was beheaded and remember considering how she might have kept it together knowing the certainty of death was so close. So I began to talk to myself in my head, think of how many people, like Anne Boleyn have had to face far worse. What about those locked away, throughout the ages, knowing they would be tortured, that no one would hear or come and save them and no one would care when tossed cold and in pain, back to their cells. Very dramatic I know but it worked. It made any anxiety about either my broader situation or that 10 minutes in a small tube a lot easier to deal with.
I was then directed to a theatre. I walked there through corridors, including workman as there was quite a bit of building work going on, holding my bag of clothes in one hand with the other grasping desperately at the hospital gown, trying to protect my modesty from behind. The little bows that canbe used to tie it up to keep it together are pretty difficult to do up given they are behind you, so essentially my bottom would most definitely have been visible had I not grasped the edges of the gown together. In the theatre there was a cubicle for my bag of clothes and the nurses indicated I should get onto the bed where they started preparing me. Smiles and politeness but I still felt rather like just another poor soul. This did not bother me, I would prefer the fit as many poor souls in this factory line efficiently than waste any more time than is necessary being too friendly. There were about 2 or 3 nurses fiddling with the machine, inserting a cannula in my arm and hooking me up to an IV of fluids, anti nausea medication and morphine. A very beautiful doctor came to check it all. I had not known quite was going to happen and was nervous. Not so much about the procedure but about the fact that Prof. Vogl would now know the extent of the spread in my liver and I could not decide if I would ask him what he could see or even if I would try and look on the screens that were visible to help him guide his work. I had wondered about the pain of the procedure also. The unexpected morphine floated through me and took away all my anxiety. It was rather lovely and I have always thought, as I did when I had a drugs prior to my generalanaesthetic a few weeks ago for the ovary removal procedure, that as long as these drugs exist perhaps the end will not be so bad. Not only can they protect you from pain but it is the mental anguish I would want to be most protected from. I decided I would neither ask him what he could see nor try and look. I worried either may result in some information that I would not be able to manage and which would haunt me daily until I returned to see if and how effective the procedure had been. I also felt that Prof. Vogl would not be a man to mince his words and preferred to have Grace as the interpreter.
I lay there for a while with nurses being busy around me and eventually Prof Vogl arrived, all gowned up. I had had antiseptic smothered over my groin area and a material cover laid over me which covered my whole body bar a window to the groin. I just looked up to the ceiling and waited as Prof Vogl injected some local anaesthetic and soon began his job, inserting a line up my femoral artery to my hepatic artery. I could not tell really what was going on but he eventually asked me if I could feel anything, for a couple of seconds I could not and then suddenly there was a whoosh of what felt like cold liquid racing around the shape of my liver - clearly he had injected the chemo. It was uncomfortable and quite a shocking sensation but quick. I am not entirely sure what he was doing next but assume this involved the embolism part of TACE - i.e. closing off the blood stream to the tumours so that they are not only poisoned by the chemo but starved of their blood supply. He had chosen to do the right lobe of the liver, which was clearly in a worse state, although my left lobe is the one I feel the most as it physically protrudes from the centre of my upper abdomen between the ribs. Perhaps it is because the right lobe is so much larger that it was key to get this under control as the liver can work relatively well even with quite a bit of it covered in tumours. The whole procedure, bar preparation and finishing up took probably less than 10 minutes.
In a later debrief with Grace (who goes through the cases with Prof Vogl , she knows and understands him and so can help interpret as well as know to ask the right questions), she said that I have substantial tumour load around the central area of the liver that is close to my stomach and aorta and we need to get this under control. Horrible words, substantial tumour load. But I am trusting that Prof Vogl is the best person in the world to get this under control if anyone can. I will have to wait a month for my next appointment at which time they will do the left lobe (unless clear that the right lobe needs more attention).
The Line in through the hepatic artery - yuch
After the procedure Prof Vogl left with few words and the nurses finished getting me ready to move. They transferred me to a trolley bed and wheeled me to a ward for 3-4 hour observation. I was not to move for this time to ensure that the femoral artery was safe and I did not start bleeding. I was still under the influence of morphine so lay there drifting in and out of sleep until my best friend came up from the waiting room to distract me and help get things like water and my book into a position that I could reach given I was unable to move. My blood pressure, temperature and pulse were taken regularly and the time went by quite fast. I was then told I could get up and leave. I had read an account from another woman who was treated by Prof Vogl of what she had called the Vogl shuffle, which I realised I now had. I basically could not lift the right leg up for 2-3 days so climbing stairs and getting into cars was a bit awkward. It was also the discomfort from where the line had gone in that bothered me most that night.
We made our way down to Prof. Vogl’s office again where they assumed I had had the post procedure CT scan. We got slightly lost in the system and hung around too long before we finally got a call for the CT scan - which took seconds. It was immediately sent to Prof Vogl who I then saw for a couple of minutes as he checked all looked ok after the procedure and I was safe to go and said he would decide what to do next when he sees the scan next time. And that was that. We made our way in a taxi to the hotel and spent the rest of the time, until the next day early afternoon, when we made our way to the airport. With all the lying around time I was able to get quite a bit of work done. It is efficient time - I can't move, I can’t be distracted and work keeps me engaged.
The following days and weeks were far worse than I had anticipated. I think I had thought that because the chemo was targeted I would feel bad for may a day or two and bounce back - but in reality I felt ok for a couple of days, but very tired and then I started feeling worse and worse. I investigated TACE more and read that this does happen. The slow release of the chemo and leakage into the system. There is also adelay for the impact of the embolism to be felt. The liver was clearly angry and felt more swollen, or at least more ‘alive’. I felt wobbly, tired, needed to rest much more than normal, out of breath - just not great for more than 2 weeks and now a good 3 plus weeks after I am finally feeling more myself. Only to prepare for round two. At least this time I will be more prepared and in the intervening time I am trying to avoid thinking about what the results might tell us about how effective it has been. It certainly feels more settled on the right, not on the left however.
I continue with my oral chemo, which I also discussed with Prof. Vogl and I have now written to my oncologist in the UK to explain my rationale for this action. My aim is to stabilise the tumours in the liver using what I consider is the most effective and targeted way to do so, which if successful will give me the opportunity I hope to start on a new hormone therapy. I continue to investigate immunotherapies and have been examining something called AIET (Autogulous immune enhancement therapy). This is available in Japan. Just as with HIV where combination therapy became to key to controlling what is now a chronic disease it feels as if we are moving to a place where this could be the key for cancer also. Combine therapies to trick the cancer and keep ahead of its mutations to keep this disease chronic not fatal. But we are so early and new approaches are bursting up all around - how the health systems will navigate their way through these to determine which are the most effective combinations for which cancers will require time and some bold thinking and risk taking. In the meantime people like me, and there are many around the world, are taking this challenge into our own hands. Money is the main obstacle but mothers who want to be alive for their children are a pretty determined lot and this makes us very resourceful. Whatever it takes to stay alive. In doing so we work with experts like Grace to navigate the old, new and even newer treatments in our quest to stay alive. In my experience each Doctor is limited by the breadth of their expertise so as science advances they cannot either keep up with all the developments, or make risky choices on behalf of their patients if they cannot be sure of the outcomes/ risks and so they stick within what they can prescribe and advise. There have been no new treatments (I lie eribulin has finally been added to the list of chemotherapies available to people with advanced breast cancer in the UK at last) - but apart from that there have been no new treatments for breast cancer for far too long in the NHS. There are treatments in the US now, routine genetic mapping of tumours which are simply so far away from being available to women in the UK that it feels criminal. The costs I know are prohibitive but with Pharmaceutical companies being even more profitable than oil companies somewhere there has to be room for negotiating prices for treatments which might actually mean they can be used to do what they were designed to do - extend and improve quality of life.
The danger is that while doctors or scientists know more and more about less and less until they eventually know everything about nothing I need to avoid ending up knowing a little about more and more until I eventually know nothing about everything.
Adapted from not sure who
The week before my visit to Professor Vogl I flew to Tanzania. I had been holding my breath that I would in fact be able to go. There were many bits of a jigsaw that needed to be in place. I needed a letter from my oncologist to say I was fit at the point of examination, for the insurance company. My appointment with him happened conveniently just before the signs of progression became very obvious. There were various hurdles to fix the meeting for the week I knew I could travel. I do not want to advertise my health issues. And I needed to stay well enough. There was quite a bit at stake had I needed to pull out, not least I would appear entirely unreliable and this important meeting that had required a number of key people to be available would have had to be cancelled with the implications of that. I was suspicious things were getting worse both after the blood test after my ovary operation which showed the inflammation marker in my liver rising to a not insignificant level and then worse, I began to feel my liver. It was at this point that I fixed my visit to Vogl for just days after my return. I was not going to panic and pull out - two fingers to the cancer I thought. How dare it disrupt me in this way. And so, with a slowly but notably swelling liver I went ahead with my plans.
Anyone who travels around Africa will know that it is one of the least well served parts of the world in terms of air travel. There are few direct flights anywhere and most routes require you to go via one of the 3 main hubs - Nairobi, Addis Ababa or Johannesburg. When I used to need to visit Malawi and Tanzania in the same visit, despite the two countries being direct neighbours the only way to fly there was to take a plane from Lilongwe in Malawi to Nairobi and from there take another plane go back on yourself to Dar es Salaam. In fact it is even more bonkers than that as the Lilongwe Nairobi route stopped in Zambia on the way - and if you look at a map of Africa you will see that Zambia is in fact in the opposite direction to Nairobi meaning you flew out of your way and then back again at least doubling the time on the plane. It would take me a whole day to make this relatively short distance. This visit to Dar es Salaam I took an Ethiopian Air flight via Addis Ababa. It was due to leave at 9pm on the Saturday, I would have a four hour stop over in Addis and then arrive in Dar around early afternoon which would get me to my hotel by around 5 or 6pm given the time it usually takes to queue and get a visa on arrival. My first work meeting was at 8am on the Monday.
We sat waiting to embark. 8.45pm and nothing. 9pm. Nothing. The flight was being not being managed by Ethiopia air staff but Star Alliance which meant that when anyone inquired what the delay was they did not seem to have the slightest clue. 10pm. Nothing. Passengers started getting a bit restless and feisty with more and more going to the desk to find out what was going on. Finally there was an announcement. The aircraft had a technical fault and engineers were trying to sort it out. Hmmm. I hoped very much it was the lights in the toilet. In fact it turned out, allegedly, to be a special screw that was missing. They needed to find out if their colleagues at British Airways had one they could use. And so we waited to find out. No. They did not and the only place they could now source this screw was from Frankfurt which meant the plane was grounded and they had to put all 300 plus of us up in airport hotels, which we finally got to around half midnight after working our way backwards through the terminal, out through immigration to pile on to waiting buses. The hold luggage was to be kept on the plane over night, so any thought of baling would be impossible - although the next day some people did which delayed us further as their bags were located and removed. In the end the flight left at 1pm the next day. A day flight was in fact much easier, I had work to finish and this would have been hard on a night flight and I would have had little time at the hotel before my first meeting had I arrived when expected. At this point I had no clue at what time I would in fact arrive in Tanzania and managed to contact the travel agent to be told I had been booked on a night flight from Addis. In practice this meant that when we landed in Addis, rather than a four hour wait a bus took those of us travelling to Dar from one plane direct to another. Rather efficient I thought - and I finally arrived in Dar in the early morning of Monday. After the visa queue I was not in bed until 3.30am. I had little sleep and wondered what all this was telling me. Travelling can be stressful. Should I be putting myself through this. I was tired but not stressed, except perhaps about my liver which was causing me discomfort. Livers do not have nerve endings so the discomfort was from the actual bulk of it pressing on my stomach and a hernia I have had since a child above my tummy button which has never given me any trouble until the last year. The work was relatively smooth. There was one slight blip when I went for a 5 minute lie down during one lunch break as I was really exhausted and needed to just close my eyes and have some time out. The next thing I knew my Tanzanian work colleague was tapping politely on my door. I had fallen deep asleep for 25 minutes. As I was the facilitator for the meeting it wasn't as if I could slip in the back door and pretend I had been doing some unavoidable really important work which had unfortunately way laid me. So I walked boldly through the front door apologising that I had been doing some unavoidable really important work which had unfortunately way laid me, looking as confident and together as I could.
Apart from the painful traffic jams in Dar on the way to the airport the return journey was more or less straight forward. A state of emergency had been declared in Ethiopia, but you would not know it waiting for 6 hours at the airport for my connecting flight home. I felt sad however. I was more tired than normal when I arrived home. I cannot pretend all is the same. I was such a physically robust person and now I feel so feeble sometimes. Accepting that life is different and will not ever look the same again is hard. Accepting the uncertainty, the changing role at work given my inability to be as physically present as I was before my diagnosis is hard. I remind myself of how lucky I am and counsel myself that this is my path now, there is no point looking back just make the most of now. Usually I am quite good at this but the trip to Dar was a concrete reminder. I used to do trips like that all the time, perhaps it was this that so starkly highlighted my reality. It was not just a normal work trip. Nothing is normal anymore.
MOre about TACE